Treating Endometriosis Infertility Naturally

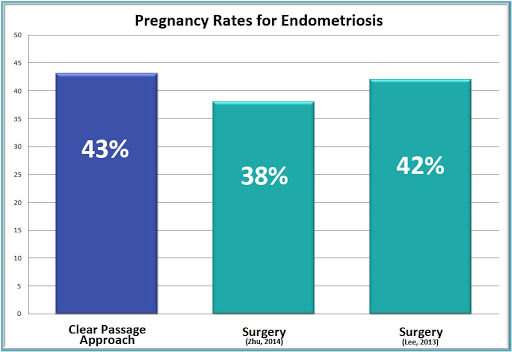
Clear Passage® is a world leader with over three decades of experience decreasing pain and improving fertility in women with endometriosis, without surgery or drugs. Initially, several peer-reviewed pilot studies examined our results treating pain and infertility in women with endometriosis. A ten-year, PubMed indexed study[i] of 1392 infertile women compared our pregnancy rates to those of surgery (see chart below). Results showed conception rates for women treated with our Clear Passage® physio/physical therapy was 43% (128/299), similar to surgical rates (38% to 49%) but without the risks of anesthesia or surgery.
Complete the online Request Consultation form to receive a free phone consultation with a therapist to learn if we may be able to help you.
Causes and Frequency of Endometriosis Infertility
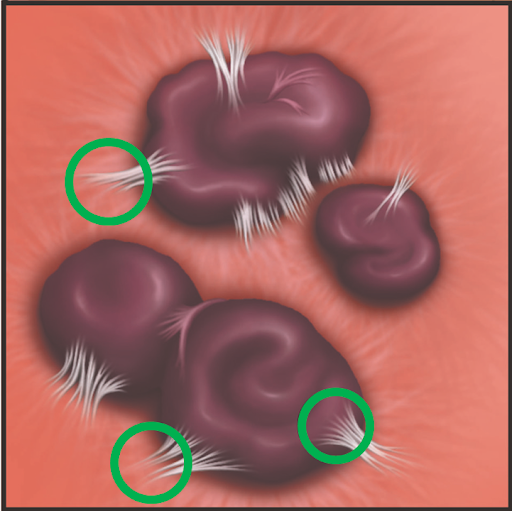
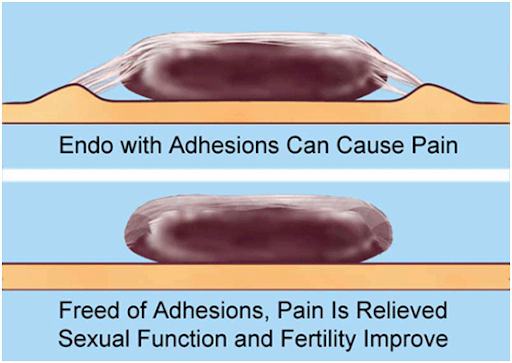
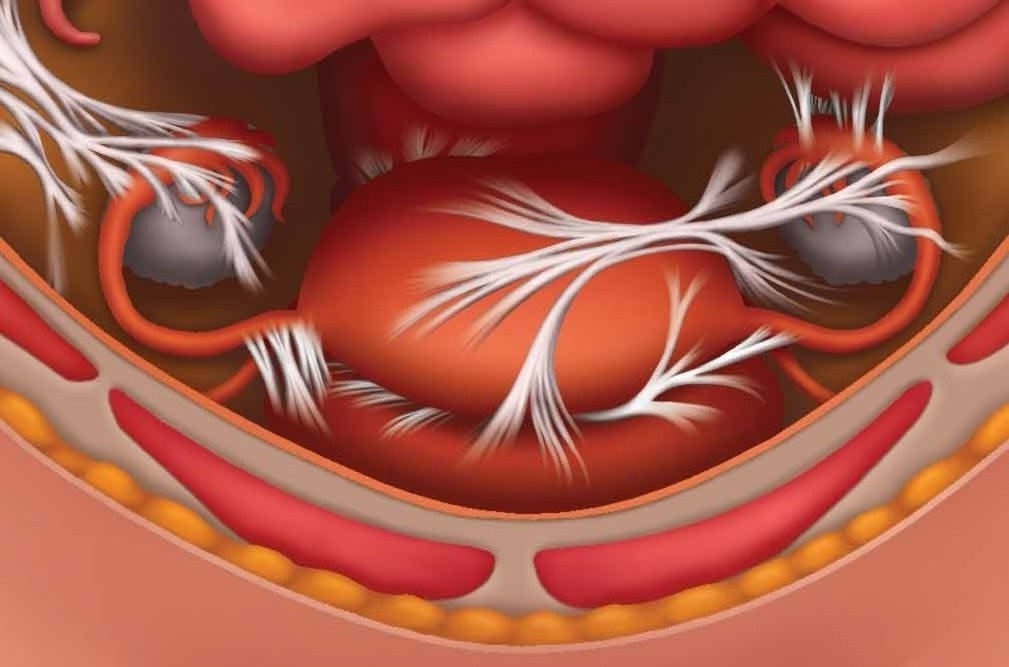
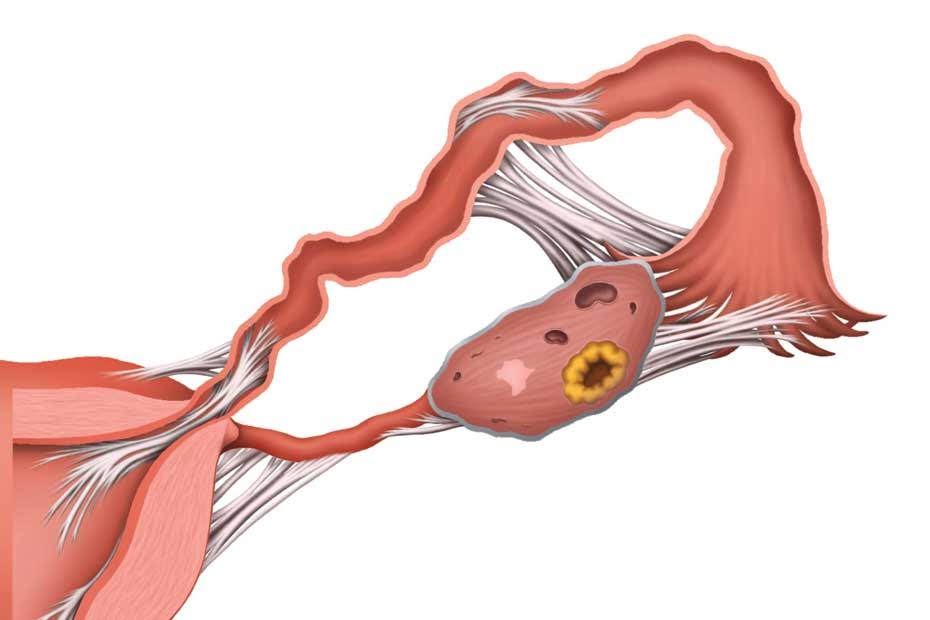
In endometriosis, tissue that normally lines the uterus is found in other areas of the body, frequently accompanied by internal bonds called adhesions. The most common areas for these misplaced tissues are on and near reproductive organs. Adhesions that form around endometrial tissue can act like an internal glue, inhibiting fertility and sometimes causing pain as they squeeze delicate structures or bind them to other structures within the pelvis.
The misplaced endometrial tissue responds to the menstrual cycle as it would in the uterus, swelling during every menstruation. But unlike menstrual fluid that leaves the body, implanted endometriosis cannot exit the body. The inflammation that accompanies the swelling can cause more adhesions to form at the site of endometrial implants, further gluing down structures that should be mobile to function properly.
How does endometriosis affect fertility?
30-40% of women with endometriosis who are trying to conceive are diagnosed with infertility.[ii] With its focus on decreasing or eliminating adhesions, the Clear Passage® approach has been used by many women as an alternative to surgery for the pain and infertility associated with endometriosis. Its use is becoming more prevalent, due to studies on our work available through the U.S. National Library of Medicine in the National Institutes of Health (NIH).
Adhesions act like glue, binding reproductive structures in curtains or rope-like bonds of collagen fibers and sometimes attaching them to neighboring structures. Bound as they are in adhesive straitjackets, the reproductive organs cannot move or function normally.
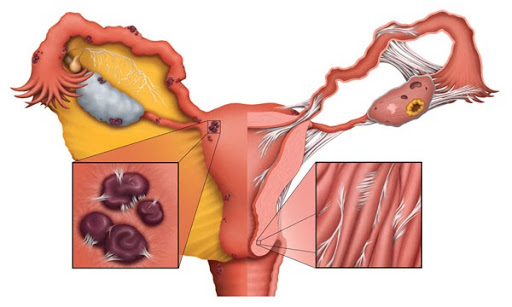
Endometrial adhesions may attach to one or both ovaries, causing ovulation pain or decreasing their ability to release an egg. Adhesions can block fallopian tubes in two ways – squeezing them closed from the outside or blocking them from the inside.
We find that endometriosis located on or near the uterus can cause uterine spasm or painful periods, decrease the opportunity for implantation, or cause miscarriage. Endometriosis which attaches to the nearby bowels may cause painful bowel movements, back, tailbone or intestinal pain. In short, adhesions within the reproductive tract can cause pain or dysfunction anywhere in the back or pelvis, including intercourse pain, and infertility.
Symptoms of Endometriosis
- Painful periods (dysmenorrhea)
- Pain during intercourse
- Pain during or after bowel movements or urination
- Excessive bleeding
- Infertility
If you are experiencing any of these symptoms along with infertility, it is quite possible you have endometriosis. The only way to identify endometriosis is with an exploratory surgery. You should speak with your doctor about the best course of action depending on the severity of your condition.
Treatments
Numerous treatment options and significant research data are available to women diagnosed with endometriosis-related infertility. Scientific data from respected medical journals allows consumers to compare the risks and success rates of various treatment options, including Clear Passage®, surgery, and pharmaceuticals. The graph on this page compares our published success rates with the published success rates of other infertility treatments for women with endometriosis – giving clear insights into options and success rates.
In a 10-year study of 1392 infertile women, the Clear Passage® approach rivaled or surpassed standard options for treating endometriosis-related infertility (surgery and pharmaceuticals) when 43% of our patients conceived after therapy. Whether used alone or as an adjunct to pharmaceuticals, many physicians were pleased to see their patients have success without surgery.
Clear Passage®️ – Treating Endometriosis and Adhesions
Adhesions have stymied Western physicians for decades. At a cellular level, they are comprised of tiny but powerful collagen fibers, similar to the strands of a nylon rope. These fibers lay down on each other in a random pattern forming a blanket or scar to surround endometriosis and nearby tissues. Once formed, they can act like glue or straitjackets in the body, causing pain or dysfunction as they bind delicate structures that should be free and mobile to work properly. Adhesions can last a lifetime and sometimes spread unless removed by us, or via surgery.
Clear Passage® staff started studying adhesions in 1984 when our physical therapist Director developed severe pelvic pain after surgery due to these internal scars. When we learned that surgery is a major cause of adhesions, our focus shifted to developing a non-surgical therapy to decrease or eliminate them.
We learned that the collagen fibers were incredibly strong; we could not break them using our hands. Then we began studying how the individual strands attach to each other. Over the years, we came to realize that we could detach these powerful strands from each other by focusing on the molecular-chemical bonds (called cross-links) that attach each strand to the next. As we developed the work, our patients’ adhesions began to dissolve and disappear. To our therapists, it felt as if we were pulling out the run in a three-dimensional sweater using just our hands.
The “hands-on” work practiced at Clear Passage® clinics is designed to reduce or eliminate adhesions, cross-link by cross-link. It has been shown to work extremely well for women with endometriosis and to have lasting effects. Many women who arrive with a history of endometriosis and infertility are now mothers of one or more children after a single five-day therapy session at Clear Passage®.
No medical techniques have 100% success rate. If you do not become pregnant soon after therapy and choose to undergo IVF, your chance for IVF pregnancy increases by 50% over IVF without prior therapy. View our success rates.
Calculate your odds with Clear Passage®️ therapy.
Other Treatment Options (Surgery, Drugs)
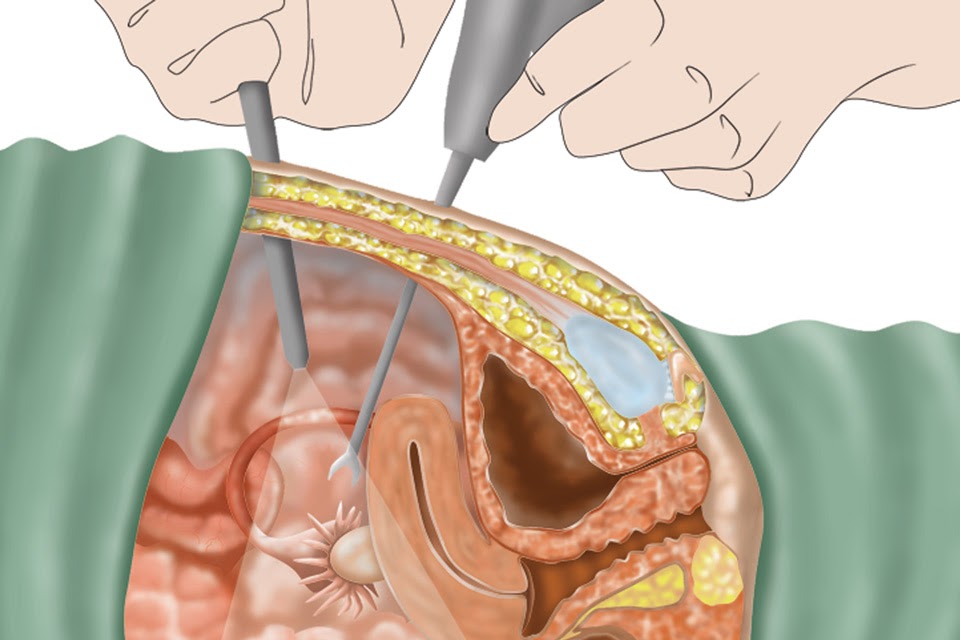
Pharmaceutical treatments for endometriosis pain generally involve hormones that prevent endometrial swelling, but also prevent pregnancy. Thus, many women with endometriosis infertility are encouraged to undergo laparoscopic surgery to burn or cut out endometriosis and any accompanying adhesions. We suggest checking your physician’s philosophy before undergoing surgery. Some are conservative; others are more aggressive. One physician told us “I can cure the endometriosis if I cut so deeply into the affected organs that I get it all.” His focus was clearly on the endometriosis, not on surgical damage to the organ.
No matter how wonderful and skilled the physician is, every surgery carries some risks, including:
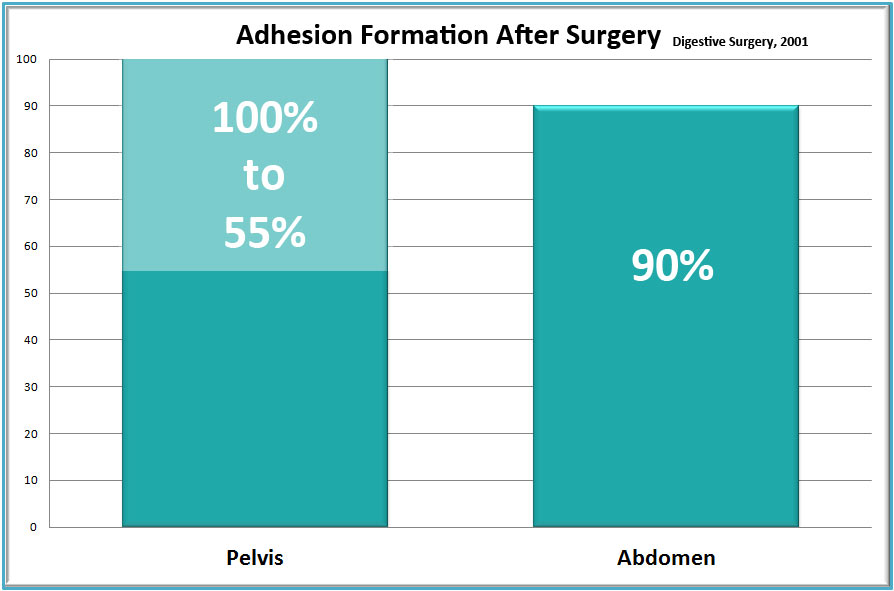
- Post-surgical adhesions. In a mammoth 58-year study of medical literature, researchers found that adhesions occur in 55-100% of women undergoing pelvic surgery.
- Risks associated with general anesthesia and infection.
- Inadvertent enterotomy (mistakenly cutting the bowel, bladder, rectum, a fallopian tube, or other structures).
Unfortunately, post-surgical adhesions can cause recurrence of pain or infertility; endometriosis tends to re-grow and spread at and around surgical sites after surgery. A study published in Fertility and Sterility found that endometriosis was most likely to re-grow in the places where it was removed during laparoscopic surgery and that unaffected regions next to endometriosis were more likely to develop endometriosis after laparoscopic surgery. [iv]
Pregnancy rates after laparoscopic surgery vary depending on the severity of the endometriosis. Women with stage I-II endometriosis experience far greater success than women with stage III-IV[v]. This is because women with stage III-IV frequently have deep endometrial implants that a surgeon cannot remove without damaging the organ or tissue. In published research, Clear Passage® pregnancy rates were shown to be equivalent or better than surgical pregnancy rates, depending on the surgery performed[vi].
Published Success Rates
To view all Clear Passage® published infertility success rates in women’s health, click here.
Treating Endometriosis Without Surgery
In the 1990s, we were surprised to find that our therapy to decrease adhesions was often decreasing pain and increasing fertility for women with endometriosis. As improvements recurred in a wide variety of women we treated, we started sharing our data with PhD researchers to design clinical trials. Beyond organizing our findings into meaningful studies, these medical researchers helped us understand the anatomical reasons our work was helping these women.
Studies on Clear Passage® Treating Endometriosis Infertility
Our first major infertility study that included women with endometriosis was published in 2004 in WebMD’s international journal Medscape General Medicine[vii]. In this pilot study of infertile women, 71% became pregnant naturally and 64% had full term deliveries. 33% of the successes reported second natural pregnancies before the study published. In addition, 67% (22/33) of women who chose to undergo IVF after Clear Passage® became pregnant after embryo transfer. We felt our work was pioneering when Medscape’s editor Dr. George Lundberg (former editor of the Journal of the American Medical Association) featured this study on the front page of Medscape’s website the month it appeared.
Several other published studies include women with endometriosis. A large study published in 2015[viii] showed a 43% (128/299) pregnancy rate for women diagnosed infertile with endometriosis. Remarkably, the success rate for opening totally blocked tubes for women with endometriosis was 60% (40/67); women with both endometriosis and totally blocked fallopian tubes had a post-therapy pregnancy rate of 38% (45/118). These results are considered extraordinary; until Clear Passage®️, no non-surgical treatment in medicine was shown to decrease pelvic adhesions or open blocked fallopian tubes. Women with endometriosis who chose to undergo in vitro fertilization (IVF) had a post-transfer pregnancy rate of 55% (31/56), which was 1.4 times the national post-transfer average during the period of the study.
Treating Endometriosis Pain
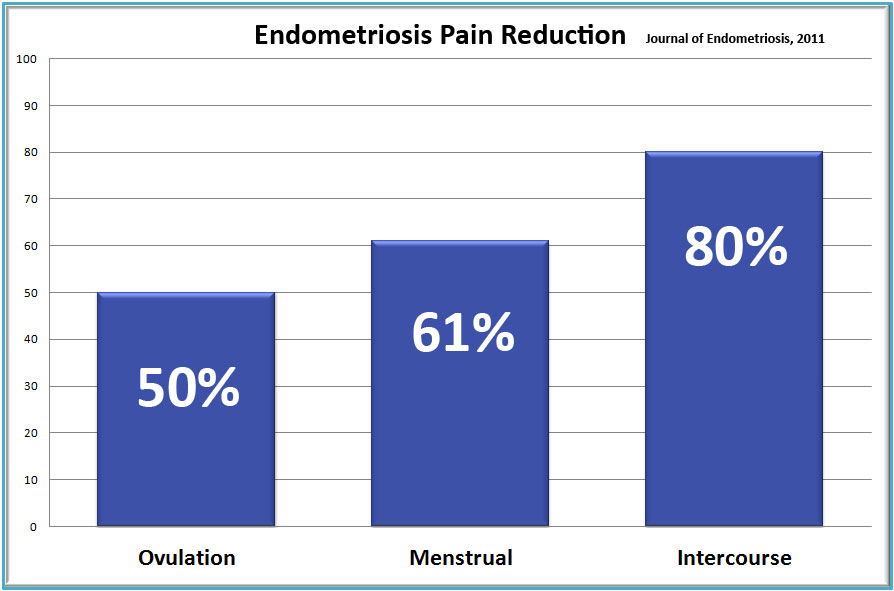
In 2004, the reproductive journal Fertility and Sterility published some of our findings in an abstract[ix] describing results of an early pilot study. In 2011, a study in the Journal of Endometriosis showed significant pain relief at all phases of the menstrual cycle and decrease in intercourse pain for women surgically diagnosed with endometriosis[x]. Reported results in the study showed:
- 80% had decreased intercourse pain
- 61% had decreased menstrual pain
- 50% had less or no ovulation pain, and
- 39% had decreased pre-menstrual pain
A follow-up report in the Journal of Endometriosis (2014) measured the long-term impact of our therapy treating menstrual and intercourse pain in women with endometriosis[xi]. The results showed that our non-surgical therapy was equivalent to surgical results twelve months after treatment, with 50% of patients reporting complete resolution of pain. This was wonderful news for women with endometriosis who were facing surgery but wanted to avoid the adhesions that so frequently follow surgical intervention.
Our Story
Clear Passage® knows pelvic adhesions well. We first faced this problem in 1984 when our founder, physical therapist Belinda Wurn, developed severe adhesions after pelvic surgery and radiation therapy for cervical cancer. Unable to work due to adhesion pain and having seen their debilitating effects in her own patients, she was determined to find a non-surgical way to decrease pelvic adhesions.
Noting the frequency of adhesions in patients with endometriosis, she and her husband, massage therapist Larry Wurn, took a much deeper look at the etiology and biomechanics of adhesion formation. They found that the chemical bonds that attached every collagen fiber to its neighbor to create adhesions appeared to dissipate when they used certain manual techniques on the adhesions. With this knowledge, they developed a unique ‘hands-on’ approach to unravel the bonds between the cross-links that comprise adhesions. They hand-picked and trained some of the most experienced manual physical therapists in the world in the methods they developed. Trained directly by the Wurns, these therapists use their non-surgical “hands-on” approach to detach the adhesions that attach endometrial implants to reproductive structures, with results cited in major medical journals. This is the same therapy we use today, with refinements we have developed since our initial inquiry, in 1984.
If you’d like a free consult, please take 20 minutes and fill out this form and we can determine if therapy would be a good fit for you.